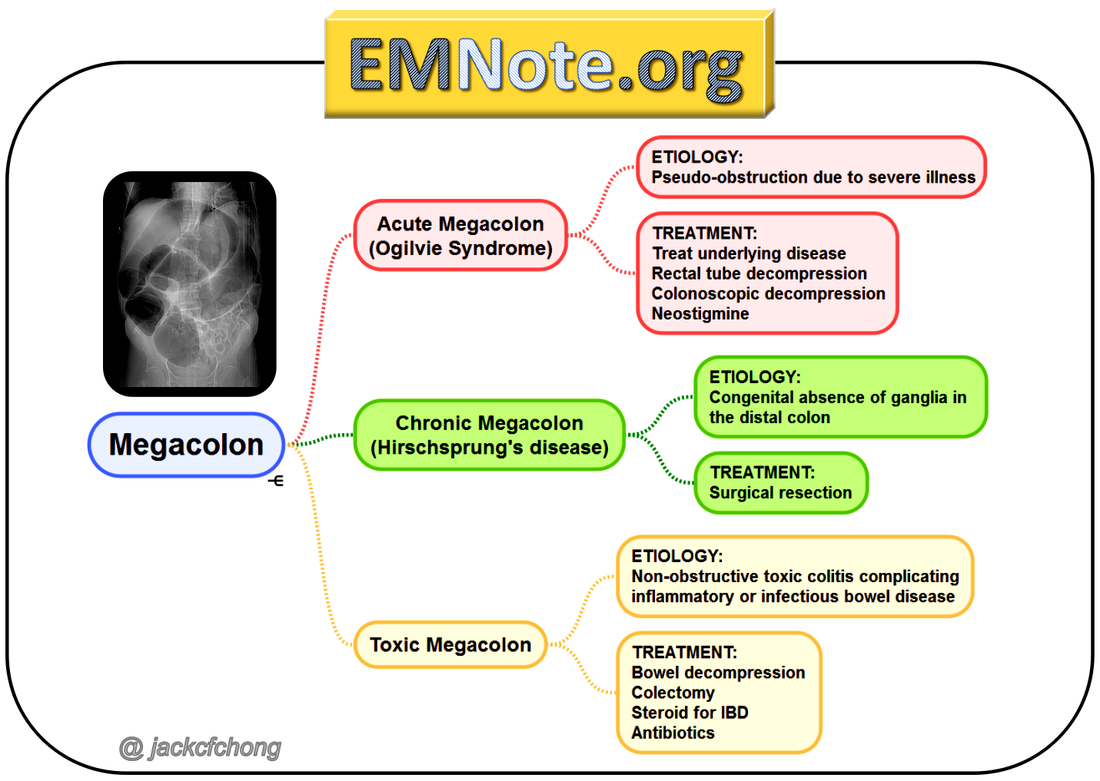
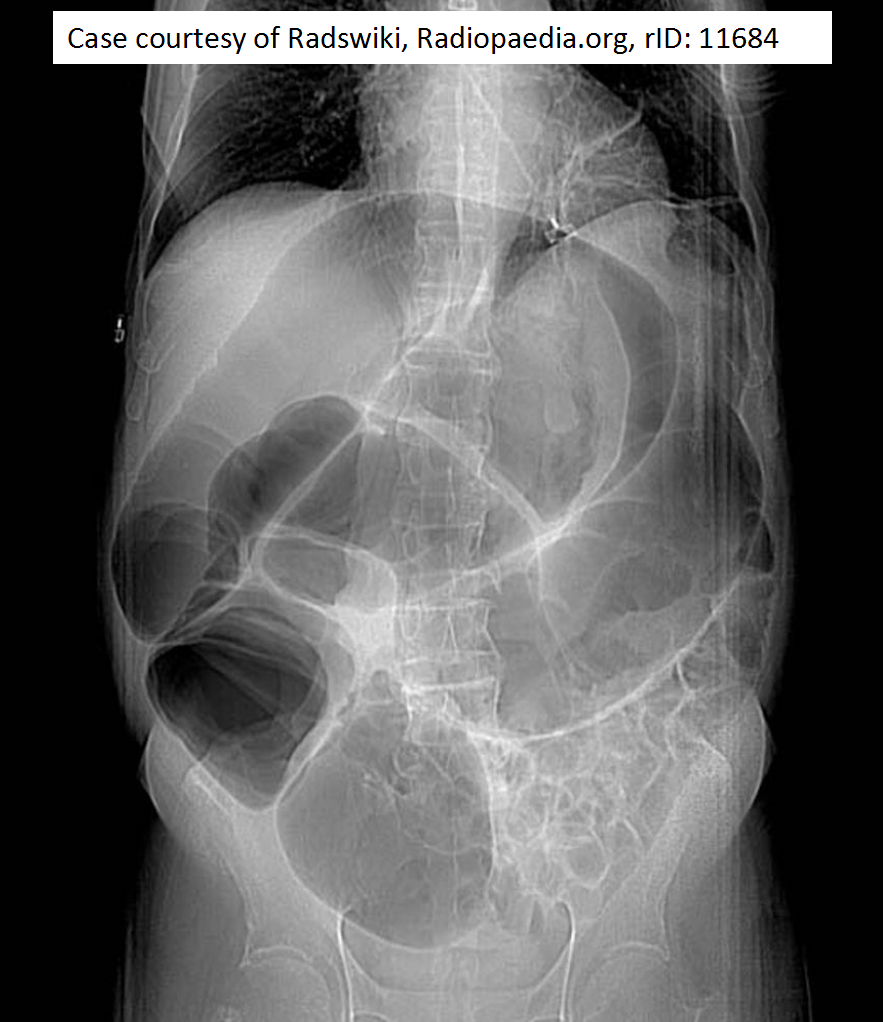
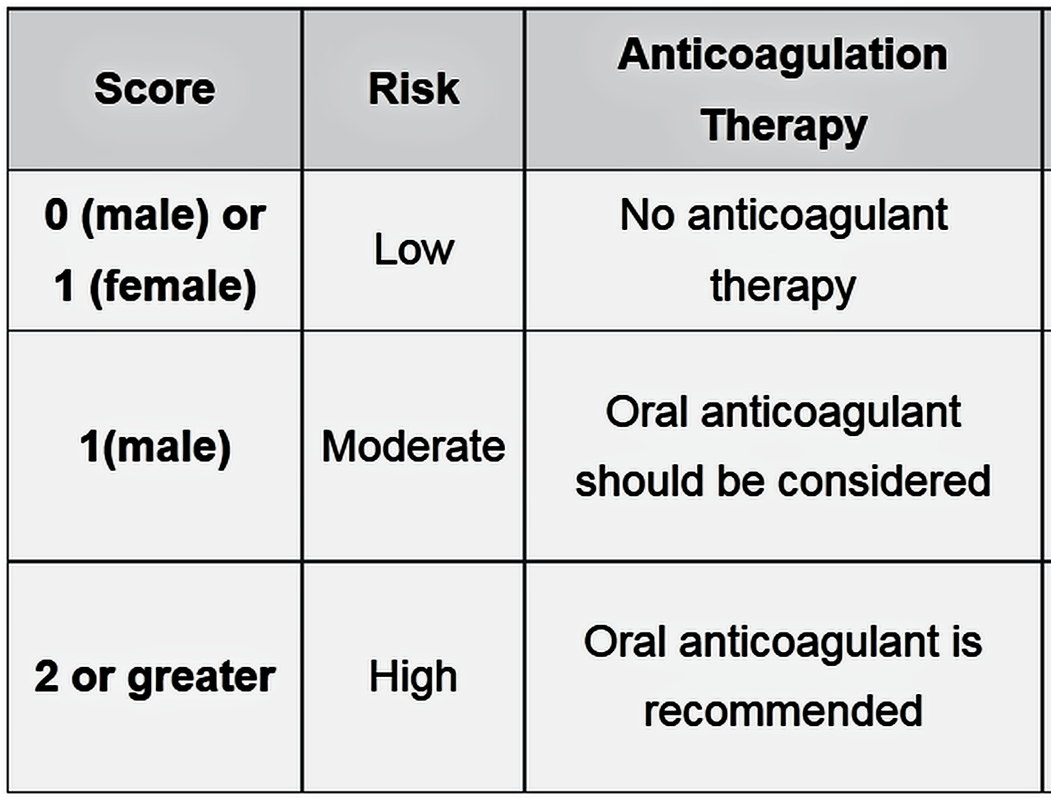
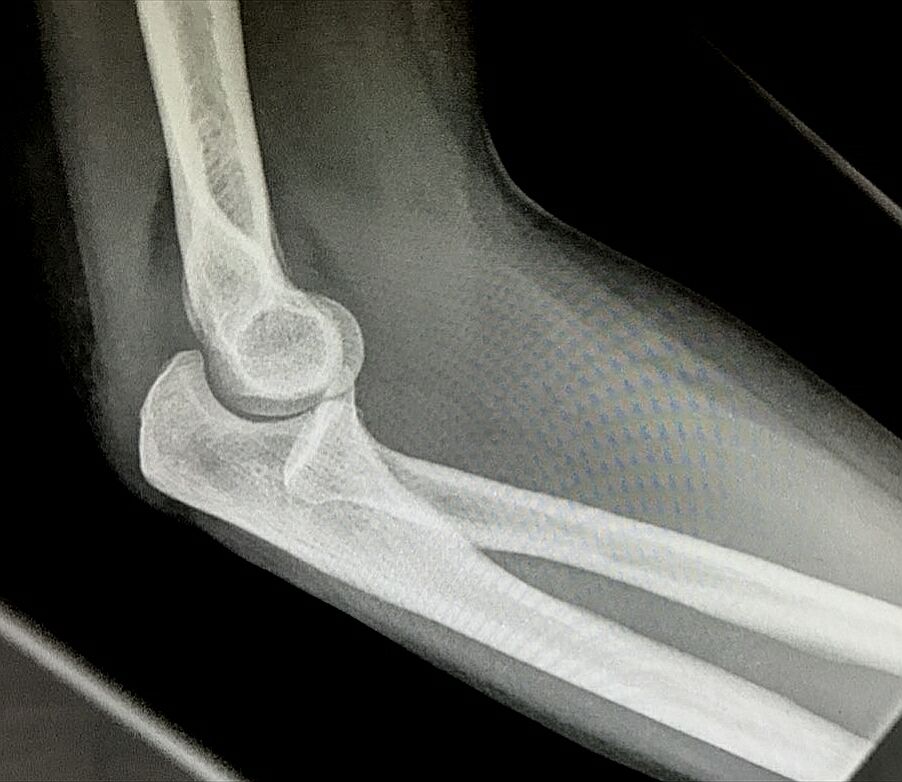
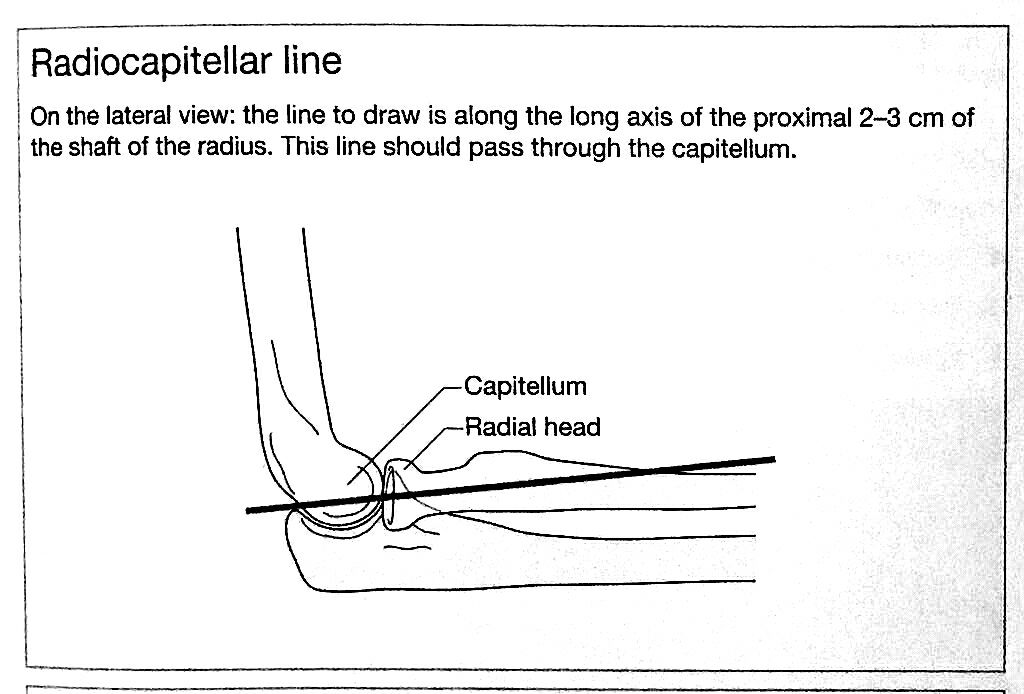
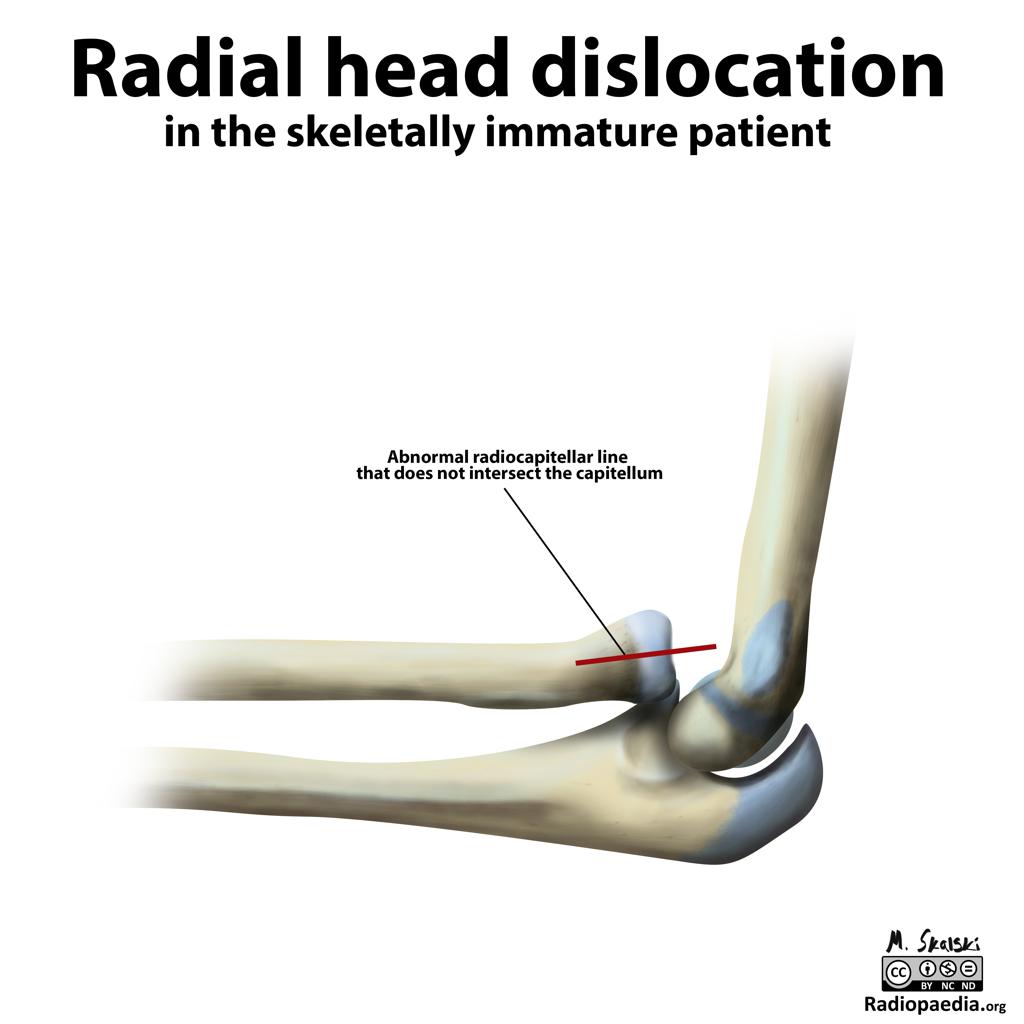
Megacolon: Acute, Toxic, and Chronic Curr Treat Options Gastroenterol. 1999 Dec;2(6):517-523. Megacolon refers to cecal dilatation above the dimension of 12 cm and above 6.5 cm of the sigmoid colon, measured at the pelvic brim. Dilatation of the colon can be broadly categorized into three clinical entities: Acute megacolon (Ogilvie's syndrome) The colonic dilatation is attributed to a sympathetically mediated reflex response to a number of serious medical or surgical conditions in elderly patients. The initial tasks are to exclude mechanical obstruction (with a hypaque enema), to discontinue enabling medications, and to correct metabolic disturbances. Dilatation of the cecum to greater than 12 cm diameter is a cause for grave concern. The rectum should be decompressed with an indwelling tube and tap water enemas. Intravenous neostigmine is generally effective and safe for patients with colonic distention unresponsive to such conservative therapies. Endoscopic decompression is necessary for patients who do not respond to, or relapse after neostigmine, or in whom neostigmine is contraindicated. Signs of peritonitis may imply colonic perforation, and surgery will be needed, often on an emergent basis. Toxic megacolon It is secondary to an identifiable inflammation of the colon. Therapy is directed toward specific treatment for the underlying disorder, inflammatory bowel disease, or infectious colitis. Bowel rest and close monitoring of the clinical status is vital. Colectomy may be needed under emergency circumstances. Chronic megacolon It may be congenital (due to Hirschsprung's disease) or may represent the end-stage of any form of refractory constipation (slow transit constipation or pelvic floor dysfunction). The initial treatment for Hirschsprung's disease is surgery, while pelvic floor dysfunction and encopresis respond to biofeedback therapy. In chronic idiopathic megacolon, medical measures, such as colonic evacuation with enemas, fiber supplementation, and laxatives may suffice. If severe motor dysfunction is confined to the colon, a subtotal colectomy with an ileorectal anastomosis, or an ileostomy may occasionally be necessary. CHA2DS2-VASc performs better than CHADS2 in predicting stroke risk. Treatment recommendations based on the CHA2DS2–VASc score are shown in the following table:
|

Author
|
Proudly powered by Weebly