|
Key points in the management of cardiac arrest in pregnancy:
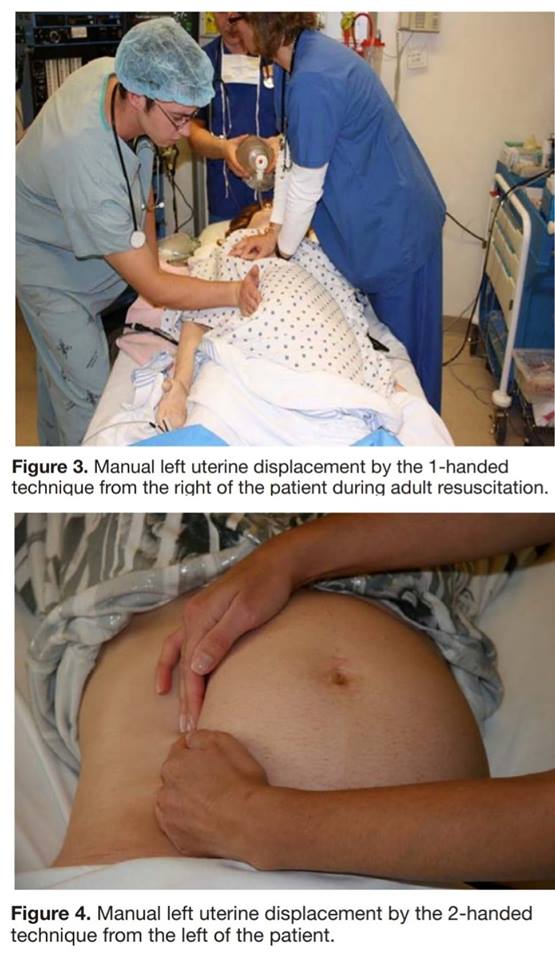
Hand location for chest compressions should be in the center of the chest as for nonpregnant patients (previous recommendations had been to shift upward to accommodate for the gravid uterus but there is no data to support this). Chest compressions should be performed with the patient supine, using manual left uterine displacement (LUD)for aortocaval decompression. Left lateral tilt position is no longer recommended due to poorer quality of cardiac compressions, the lack of full aortocaval decompression, and further complication of other procedures such as airway management. IV or IO access should be obtained above the diaphragm, to ensure no interference to flow to the heart by the gravid uterus. Rate and depth of chest compressions, ACLS drugs and doses, and defibrillation all remain the same as in nonpregnant OHCA patients. NB: As opposed to nonpregnant patients periarrest, oxygen saturation in the pregnant female should be maintained at 95% or greater, or PaO2 > 70 mmHg, to ensure appropriate oxygen delivery to the fetus. The goal PCO2 is ~28-32 mmHg, to facilitate fetal CO2 removal. If advanced airway is pursued, the most experienced provider should perform intubation due to the higher intrinsic difficulties, more rapid decompensation, and propensity for airway trauma and bleeding in the pregnant female. Perimortem c-section should occur within the first 5 minutes of cardiac arrest / arrival to the ED in ongoing arrest. Circulation. 2015;132:1747-1773. DOI: 10.1161/CIR.0000000000000300 https://umem.org/educational_pearls/3556/ Comments are closed.
|

Author
|
Proudly powered by Weebly