|
Morel-Lavallee Lesion
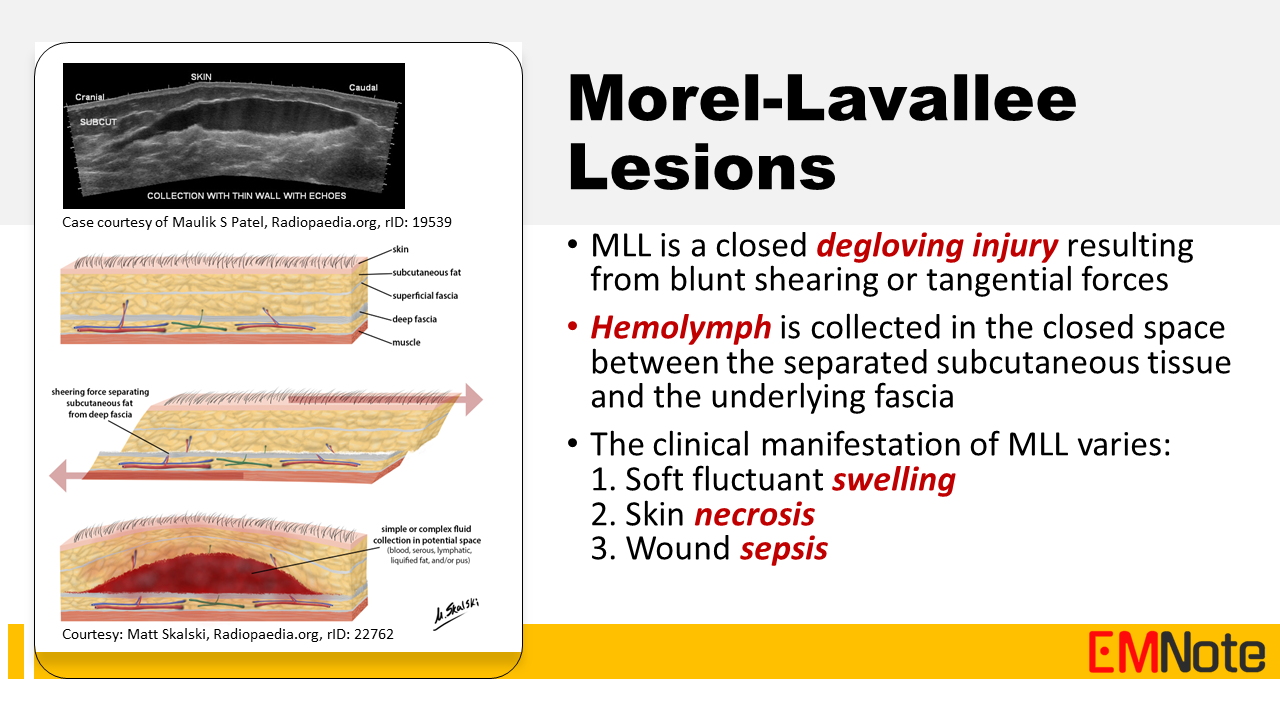
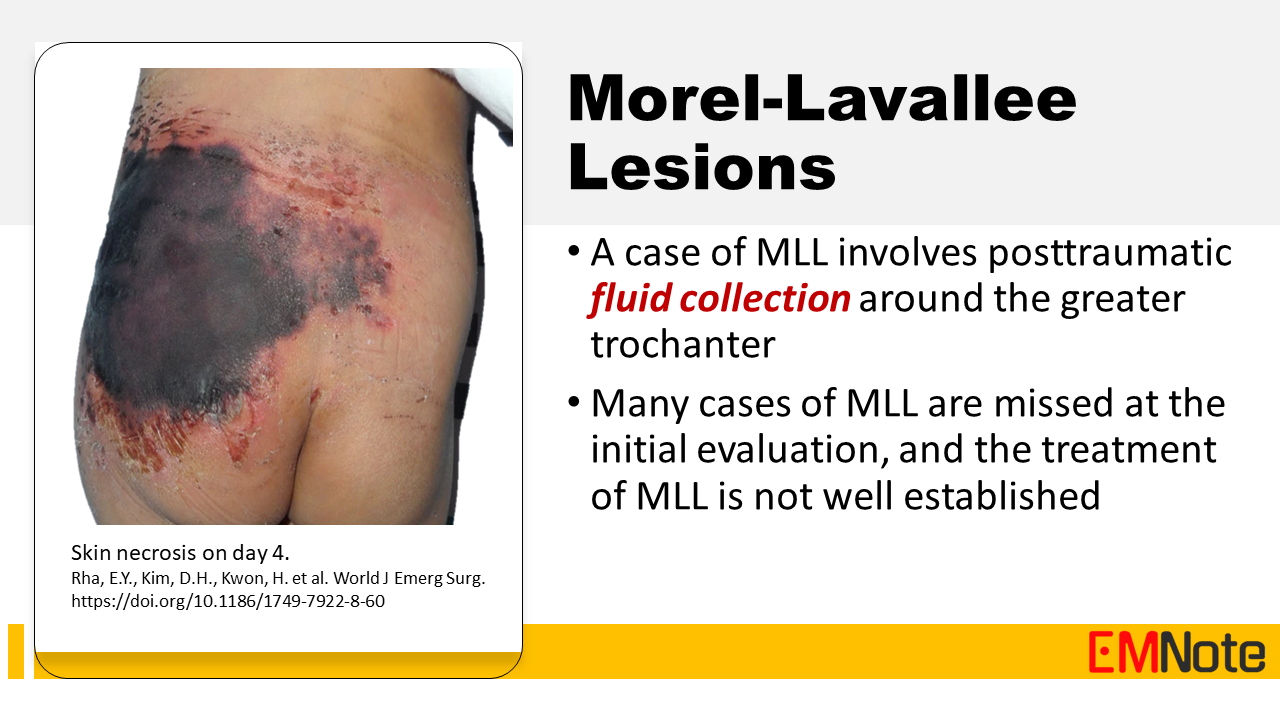
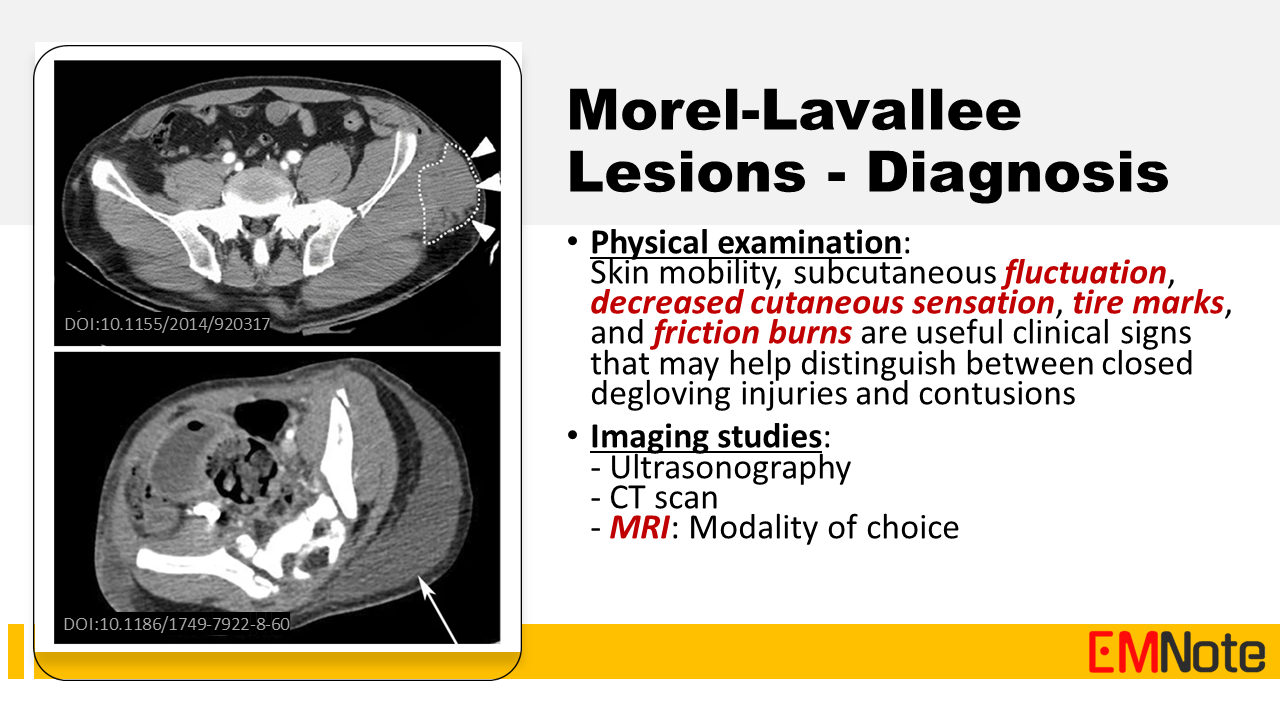
Background Morel-Lavallee lesion (MLL) is a closed degloving injury resulting from blunt shearing or tangential forces. In this condition, hemolymph is collected in the closed space between the separated subcutaneous tissue and the underlying fascia. MLL is associated with a potential risk of skin necrosis and soft tissue infection. Its clinical manifestation varies from soft fluctuant swelling to skin necrosis or wound sepsis. Physical examination Physical examination findings that may help distinguish between closed degloving injuries and contusions include: skin mobility, subcutaneous fluctuation, decreased cutaneous sensation, tire marks, and friction burns. Imaging studies for MLL include: Ultrasonography, CT scan, and MRI. MRI is the imaging technique of choice due to its superior soft tissue resolution and ability to identify the presence or absence of a capsule surrounding the fluid collection, which guides treatment decisions. Management Management of Morel-Lavallee lesions depends on several factors, including the size, location, and presence of complications. Nonoperative treatment with compression dressings, observation, and pain management is often sufficient for smaller lesions. However, larger or symptomatic lesions may require percutaneous aspiration or open surgical debridement to remove the fluid collection and prevent complications. Take Home Message Given their potential to mimic other conditions and contribute to surgical site infections, Morel-Lavallee lesions should be considered in the differential diagnosis for trauma patients presenting with soft tissue swelling, particularly in the prepatellar or hip regions. Early diagnosis and prompt initiation of appropriate management, including timely referral for definitive imaging and intervention, are crucial to prevent long-term complications and optimize patient outcomes.
0 Comments
Leave a Reply. |

Author
|
Proudly powered by Weebly