|
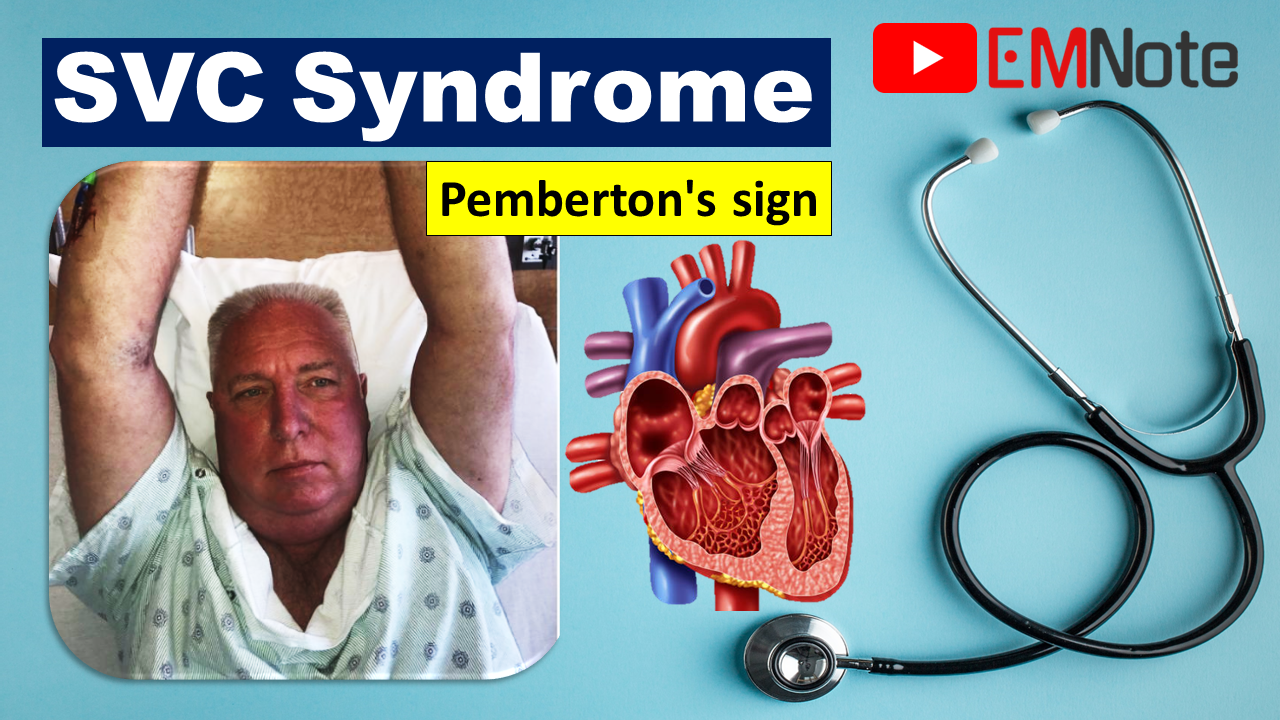
Superior Vena Cava Syndrome
2 Comments
12/4/2023 03:45:54 pm
https://turkeymedicals.com/medical
Reply
2/6/2024 04:12:11 am
However, there is no specific Islamic prayer or wazifa mentioned in the Quran or Wazifa to cure muscle weakness directly.
Reply
Leave a Reply. |

Author
|